Sharing data for cancer research
NSCLC
Data from: Survival prediction of non-small cell lung cancer patients using radiomics analyses of cone-beam CT images
Data from: Prognostic value of blood-biomarkers related to hypoxia, inflammation, immune response and tumour load in non-small cell lung cancer – a survival model with external validation
Prognostic value of blood-biomarkers related to hypoxia, inflammation, immune response and tumour load in non-small cell lung cancer - a survival model with external validation
Aim: Improve the prognostic prediction of clinical variables for non-small cell lung cancer (NSCLC), by selecting from blood-biomarkers, non-invasively describing hypoxia, inflammation and tumour load.
PET-based dose painting in non-small cell lung cancer: Comparing uniform dose escalation with boosting hypoxic and metabolically active sub-volumes
A validated prediction model for overall survival from Stage III Non Small Cell Lung Cancer: towards survival prediction for individual patients.
Purpose: Although homogeneous according to TNM staging system, stage III NSCLC patients form a heterogeneous group, which is reflected in the survival outcome. The increasing amount of information for an individual patient and the growing number of treatment options facilitate personalized treatment, but also complicate treatment decision making. Decision Support Systems (DSS), providing individualized prognostic information, can overcome this, but are currently lacking. A DSS for stage III NSCLC requires development and integration of multiple models.
Prognostic value of metabolic metrics extracted from baseline positron emission tomography images in non-small cell lung cancer
BACKGROUND: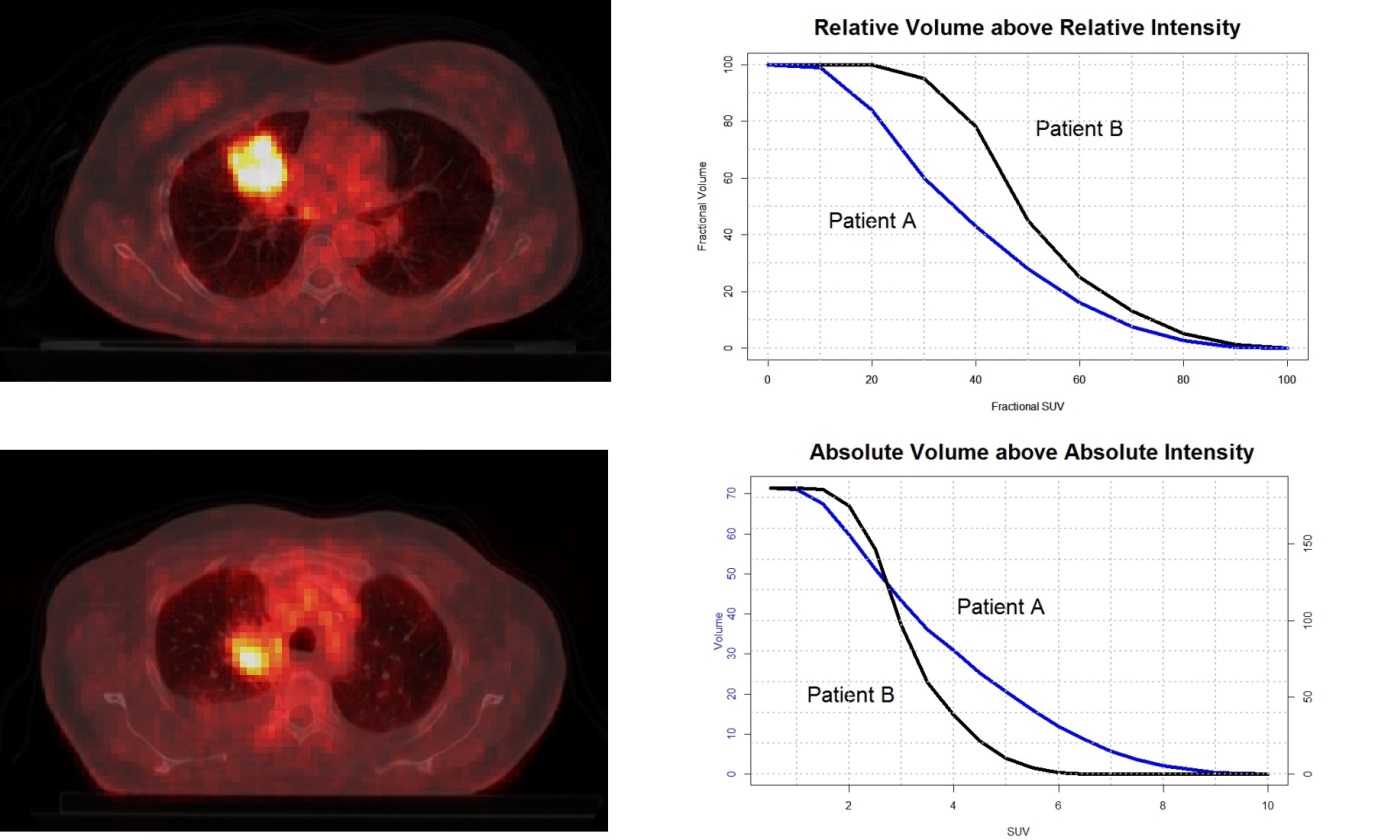
Maximum, mean and peak SUV of primary tumor at baseline FDG-PET scans, have often been found predictive for overall survival in non-small cell lung cancer (NSCLC) patients. In this study we further investigated the prognostic power of advanced metabolic metrics derived from intensity volume histograms (IVH) extracted from PET imaging.
Decoding tumour phenotype by noninvasive imaging using a quantitative radiomics approach
Human cancers exhibit strong phenotypic differences that can be visualized noninvasively by medical imaging. Radiomics refers to the comprehensive quantification of tumour phenotypes by applying a large number of quantitative image features.
EuroCAT Umbrella Protocol for NSCLC
For the EuroCAT project, a research protocol that describes a standardized data collection for non-small cell lung cancer was written and has been approved by the Medical Ethical Board of our hospital. A copy of the protocol and the appendices, including scoring of side effects, quality of life questionnaires and optional biobank procedure can be downloaded below.
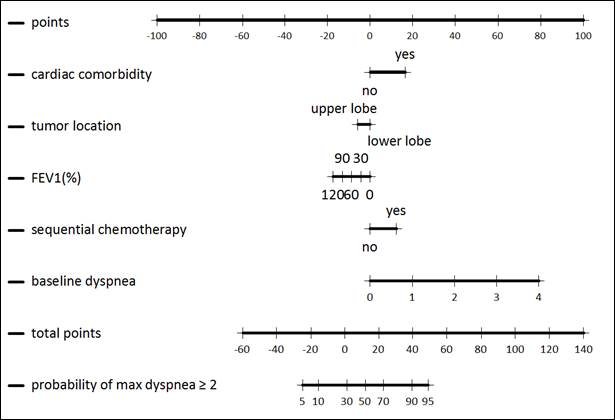
Cardiac comorbidity is an independent risk factor for radiation-induced lung toxicity in lung cancer patients
Purpose: To test the hypothesis that cardiac comorbidity before the start of radiotherapy (RT) is associated with an increased risk of radiation-induced lung toxicity (RILT) in lung cancer patients.